HPV
Human papillomaviruses (HPV) are a very common group of viruses that infect epithelial tissue.
- More than 200 HPV types have been identified.
- At least 14 types of HPV have been found to cause cancer and 70% of all cervical cancers are caused by HPV types 16 and 18.
- HPV infection is also associated with oropharyngeal and anogenital cancers (cancers of the mouth, throat, anus and genitals).
Transmission
- HPV is transmitted through contact with infected genital skin, mucous membranes (such as eyes, mouth and nose), or body fluids, and can be transmitted through sexual contact.
- It can live in the external environment for long periods and is highly transmissible.
- Approximately 80% of all sexually active individuals will be infected at some point in their life.
- Most persons get infected with HPV the first time they have sexual intercourse.
Disease Burden
- In Jamaica, HPV prevalence studies (2010) found that HPV types 16 and 18 were present in 10.5% of the general population and in 71% of women with abnormal Pap smears.
- Cervical cancer is the second leading cause of cancer-related death in the world and in Jamaica. It remains a significant public health concern.
- Current estimates indicate that every year in Jamaica 392 women are diagnosed with cervical cancer and 185 die from the disease.
HPV Vaccine
- HPV vaccines are recombinant vaccines. There are no live viruses or viral particles in these vaccines.
- There are 3 HPV vaccines currently available: bivalent (2-valent), quadrivalent (4-valent) and nonavalent (9-valent). The HPV types covered by these vaccines are outlined in the diagram below:
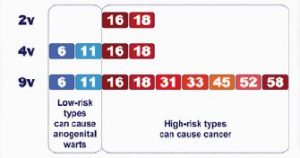
- All 3 HPV vaccines protect against HPV types 16
and 18.
HPV Vaccine Recommendations
- The World Health Organization (WHO) recommends that HPV vaccines be included in national immunization programmes as a core strategy for primary prevention against cervical cancer. The WHO states that HPV vaccination for 9–14 year-old girls is the most cost-effective public health measure against cervical cancer.
- HPV vaccination in Jamaica is part of a coordinated and comprehensive approach to cervical cancer control that also includes secondary prevention through screening (such as Pap smears) and treatment of adult women for pre-cancers, and tertiary and palliative care for women affected by cervical cancer.
- The Ministry of Health introduced the bivalent HPV vaccine to Grade 7 girls in October 2017 to provide the best protection against HPV types 16 and 18.
HPV Vaccine Safety
- HPV vaccines are very safe.
- Side effects following HPV vaccination are mild and may include redness, swelling or tenderness at the injection site.
- The Global Advisory Committee on Vaccine Safety (GACVS) investigated concerns related to anaphylaxis (severe allergic reactions), syncope (fainting), mass psychogenic illness, autoimmune
diseases, including multiple sclerosis and Guillain-Barré syndrome and thromboembolism and each was confirmed as not related to HPV vaccination. - HPV vaccines should not be given to anyone who has had a severe allergic reaction after a HPV vaccine dose, or to a component of the vaccine.
HPV Vaccine Effectiveness
The three registered vaccines (2, 4 and 9-valent) offer relatively similar effectiveness for the prevention of cervical cancer caused by HPV types 16 and 18. More than 70 countries around the world have introduced the HPV vaccine and many of them have observed significant reductions in the occurrence of HPV infections and cervical pre-cancers in their population where uptake of the vaccine is high.
- It is not necessary to screen for HPV infection prior to HPV vaccination.
- Achieving high vaccination coverage in girls (>80%) reduces the risk of HPV infection in boys due to the ‘herd immunity’ effect.
- The vaccine is best administered before the onset of sexual activity for optimum protection, i.e. before first exposure to HPV infection The immune response to the vaccine is also best when given at a young age.
Cervical cancer screening is recommended for women whether or not they have been vaccinated.
HPV Vaccination Schedule
WHO recommends a 2-dose schedule for those 9–14 years of age, with a 6-month interval between the first and second doses. Those ≥15 years of age at the time of the second dose
are adequately covered by 2 doses. There is no maximum recommended interval between doses. However, an interval no greater than 12–15 months is suggested to complete the schedule. If the interval between doses is shorter than 5 months, a third dose should be given at least 6 months after the first dose.
A 3-dose schedule (0, 1–2, 6 months) should be used for all vaccinations initiated ≥ 15 years of age and in those younger than 15 years known to be immunocompromised (weakened immune system).
Contact
Please contact the Ministry of Health at 1-888-ONE-LOVE (663-5683) [email protected] or your nearest health centre for more information.
References
Click here to view all references.



